|
If the diagnosis of cardiac arrest is uncertain, initiating CPR is preferable to withholding CPR.Prioritize airway and breathing (i.e., ABC approach) for cardiac arrest secondary to respiratory arrest.For sudden cardiac arrest, use the CAB approach to begin chest compression as soon as possible.This involves neuroprotective measures, hemodynamic support, critical care admission, monitoring for organ dysfunction, and treatment of underlying causes and complications. Modifications to BLS and ACLS are required for children and neonates.Īfter the return of spontaneous circulation ( ROSC), comprehensive postresuscitation care is essential for good neurological and functional outcomes. ACLS includes additional measures (e.g., resuscitation medications, airway management) and identifying and treating reversible causes of cardiac arrest (e.g., Hs and Ts). BLS involves checking responsiveness, calling for help, performing chest compressions and rescue breaths, and, if available, using an automated external defibrillator ( AED). There are two clinical algorithms to provide CPR: basic life support ( BLS) for lay rescuers and medical professionals alike and advanced cardiac life support ( ACLS) solely for medical professionals. Immediate initiation of high-quality chest compressions is the most important factor for survival after cardiac arrest. 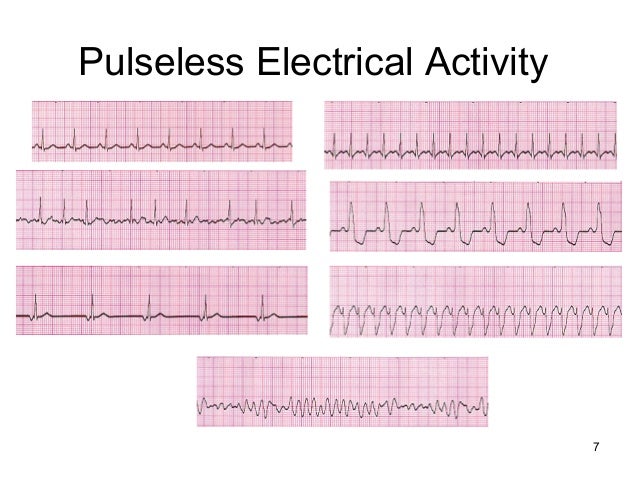 
Cardiopulmonary resuscitation ( CPR) is a lifesaving procedure that artificially maintains circulation and ventilation until cardiac function is hopefully restored. In adults, cardiac arrest is most commonly caused by cardiac conditions (e.g., coronary artery disease), but it can also have noncardiac etiologies (e.g., hypothermia), whereas in children, etiologies are more varied and more frequently related to profound hypoxia (e.g., due to airway obstruction). An impalpable pulse should not always be taken as a pulseless electrical activity because it may be due to severe peripheral vascular abnormality.Ĭopyright © 2023, StatPearls Publishing LLC.Cardiac arrest is the sudden cessation of cardiac function and blood circulation, manifesting as apnea, pulselessness, and loss of consciousness. Pulseless electrical activity can include a number of organized cardiac rhythms that may be supraventricular in origin, sinus versus non sinus, or ventricular in origin such as accelerated idioventricular or escape. True pulseless electrical activity is a state in which cardiac contractions are lacking in the presence of coordinated electrical impulses. There can be ventricular contractions and detectable pressures in the aorta, which are also known as pseudo-PEA. Pulseless electrical activity does not necessarily mean the lack of mechanical activity. The word “sufficient” is being used to describe a degree of ventricular mechanical activity that is adequate to generate a palpable pulse. In the case of cardiac arrest, the organized ventricular electrical activity does not usually follow sufficient ventricular response. It means that the electrical activity is pertinent, but not sufficient, condition for contraction. 
A lack of ventricular impulse often points to the absence of ventricular contraction, but the contrary is not always true. Pulseless electrical activity (PEA), also known as electromechanical dissociation, is a clinical condition characterized by unresponsiveness and impalpable pulse in the presence of sufficient electrical discharge.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
